The Slow Creep of Stress: What a Recent MS Flare-Up Reminded Me About Boundaries, Burnout, and the Body’s Quiet Warnings
- Carlita L. Coley

- Jul 21
- 6 min read
Updated: Jul 24
It started with a simple morning stroll to stretch my legs, and clear my mind. I had been holding so much tension in my body without even realizing it. But by the time I made it back inside, something was off. A strange, unfamiliar tightness settled in the center of my chest and as the hours passed, it didn't go away. It grew. At first, I brushed it off. Maybe I was just tired, or overthinking things, the way I sometimes do when stress lingers in my body longer than it should. I took two Tylenol, laid down, and waited for the feeling to pass. But the pressure lingered, and with each breath, I realized something wasn’t right.
I wondered if it could be anxiety, but even that didn’t fully add up. I was carrying more emotional and physical strain than usual, yes, but I didn’t feel panicked. I didn’t feel overwhelmed, at least not in the spiraling way we often associate with anxiety attacks. Like many of us do, I turned to Google. The symptoms I read mimicked those of a heart attack, and suddenly, it became clear: this wasn’t something I could afford to ignore. In the end, it was the uncertainty that pushed me to seek care.
Seen and Safe
By early afternoon, I found myself sitting in the emergency room, exhausted, lightheaded, short of breath, and still feeling that persistent ache in my chest. And if I’m being honest, I was a little scared. I'm not a fan of hospitals; they aren’t really my thing. I’m the type who second-guesses whether something is “serious enough” for an ER visit. But the pressure wouldn’t let up, and I knew I couldn’t ignore it.
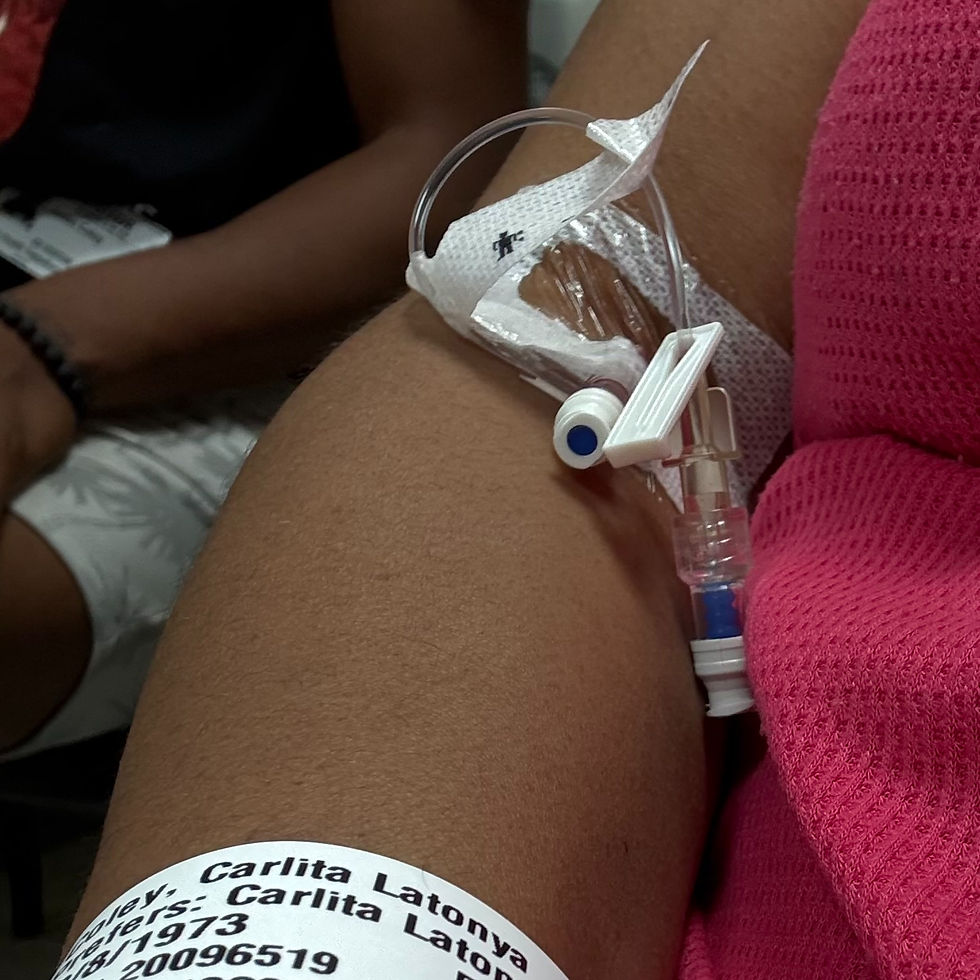
When the nurse called me back, she asked me to describe what I was feeling. It wasn’t easy—every word felt like it pulled the air right out of me, but I explained the tightness, the pressure, the fatigue. She listened, then placed the little EKG tabs across my chest and got to work checking vitals.
No one mentioned Multiple Sclerosis(MS) at first—not until the doctor came in. He’d looked over my chart and gently asked if I’d ever had a flare-up like this before. I told him no, because honestly, it hadn’t even crossed my mind that this could be connected to my MS. He explained that MS can be unpredictable and that flare-ups can show up in all kinds of ways. As a precaution, he recommended a steroid treatment, noting that even if it wasn’t a flare, the stress alone could trigger one—and treating early could still make a difference.
But what I appreciated most was that he didn’t stop there. He ordered all the tests—CT scan, blood work, another EKG—just to be sure we weren’t missing something more urgent. That balance of validating my experience while still being thorough made me feel seen, and more importantly, safe.
While waiting for results, I sent a few texts to close friends and family. Not because they could fix anything, but because it helped to know someone else knew what I was facing. One friend, who always shows up without being asked, even came to the hospital. Just having them nearby meant more than I can say. It reminded me that even in the scariest, most vulnerable moments, I don’t have to carry it all alone.The test results eventually came back normal; no signs of a heart attack, blood clots, or anything that pointed to a cardiac crisis. The doctor reassured me that my heart looked strong and healthy, though he still encouraged me to follow up with a cardiologist, just to be safe.
Based on my symptoms, the timing, and how quickly I responded to the steroid treatment, the doctor explained that what I was likely experiencing was a neurological flare consistent with MS. That’s when I first heard the term “MS hug.” The MS hug is a symptom of Multiple Sclerosis that feels like a tightening or squeezing sensation that wraps around the chest or torso, like a pressure band that refuses to let go. For some, it’s mildly uncomfortable. For others, like me yesterday, it can be sharp, breath-stealing, and deeply unsettling. It’s not dangerous in the way a heart attack is, but it is your nervous system misfiring, sending confused signals to your body. And in my case, it was also my body’s way of raising a red flag, trying to get my attention after too much buildup for too long.
My experience with the MS hug revealed how layers of quietly filed away stress, grief, and emotional labor can accumulate into something deeply physical. I’d been carrying so much in the weeks leading up to yesterday: the grief of recent losses, the weight of caring for others, the mental load of trying to do and be all the things. None of it felt urgent at the time. But in that ER room, my body spoke what my mind had been trying to downplay. The stress I’d been holding had finally demanded a voice, and it chose a flare-up to do the talking.
A Call to Reconnect
I’ve spent years reading, writing, teaching, and even living the principles of self-care, boundaries, and rest. They’re not new to me. But every now and then, life will hand you a moment that makes you revisit those very lessons because something about your current season demands that you apply them more intentionally than before. It was a call to reconnect with the things I already knew to be true and to practice them even in the more challenging moments. It was a reminder that:

Self-care is not selfish; it's a stabilizer. Somewhere between constantly giving and completely shutting down, there's a middle ground. I've come to understand self-care as that balance point—a daily practice that helps me recalibrate so I can continue showing up, but from a place of wholeness. It’s not about bubble baths or checklists—it’s about learning what restores me and letting that be enough.
Rest is more than sleep. True rest isn’t just physical stillness—it’s quieting the mental spin, easing the emotional labor, letting your nervous system take a breath. I've learned that sometimes, “doing nothing” is actually doing everything my body and spirit need in that moment. Rest is not lazy; it's intentional, productive healing.
Boundaries are anchors. Setting limits honors what I need to feel safe, grounded, and sane. Boundaries aren’t about controlling others, it's about focusing on the things I can control, which is staying in integrity with myself. I can’t dictate other people’s behavior, but I can decide what I will and won’t allow in my space.
Permission to pause is a radical act of care. There’s so much messaging about pushing through, grinding harder, doing more. But I've had to learn that stopping isn’t failure—it’s wisdom. Giving myself permission to step back, reassess, or simply breathe has been one of the
most important ways I’ve preserved my mental and physical health. It’s how I protect my capacity to continue.
MS and Stress Worth Tending To
This flare-up was a painful reminder is that my body is messenger, and it won’t let me bypass what needs to be addressed, or let me grind through emotional weight without consequence. While I’ve always understood that conceptually, experiencing it physically brought the lesson home in a new way. Stress doesn’t always shout; sometimes it whispers, quietly stacking up in the background, until one day your body takes over and says, “enough.” MS is unpredictable. And life doesn’t always slow down when you need it to. So now, I’m going to listen to my body more closely and better tend to myself, even when it's not convenient. I plan to be more intentional and present, finding ways to pace myself differently: to rest without guilt, to recalibrate when things shift, and to treat stress as something worth tending to. Not just when it reaches a crisis point, but as a regular practice of my melanin wellness.





Comments